Good communication exerts positive influence on the emotional health of a patient as well as symptom resolution, functional and physiological status, and pain control. Effective physician-patient communication is a critical component to the relief of your patients’ health ailments.

Medicate or communicate?
You thought medications did the trick right? Yet efficacious communication with your patient has been validated through research as to its potency in its ability to speed patient’s recovery. The issue: doctors and patients do not agree on the degree of communication skills present. It is two separate worlds of thought in terms of how doctors think they are communicating with their patients and how their patients perceive it to really be.
Agreement between both parties in regards to the nature of the problem and the course of action appears to aid in developing a more positive perception. As a physician, you should attend to the patients problems as a whole and take his/her expectations into account; this is described as “illness experience” during history taking (Stewart, 1995). Once a diagnosis is reached and a management plan has been conjured it is critical to give clear information and find common ground.
In a recent analysis of doctor-patient relationships by David A. Kenny, et al, they found four very interesting results:
-
Doctors tend to perceive themselves to be more alike from one patient to another patient than patients perceive them to be.
-
From one doctor to another, doctors tend to see themselves quite differently but patients do not.
-
Patients of the same doctor do not agree very much with each other about level of communication skills of their doctors.
-
Some doctor’s scores did not correlate better with their patient’s scores of their communication skills than with scores received by other doctors.
It is as if no one is seeing eye to eye! To remedy reassure your patient that you care and are empathetic towards their needs, this has a very profound effect on their well-being. A systematic review of 25 years of research has found that (Stewart, 1995):
-
50% of psychosocial and psychiatric problems are missed
-
Physicians interrupt patients on average of 18 seconds into their description
-
54% of patient problems and 45% of patient concerns are neither elicited by the doctor nor disclosed by the patient
-
In 50% of visits, the doctor and patient do not see eye-to-eye on the main problem
-
Patients are overall dissatisfied with information provided by the doctor
Complete Patient History is Critical

Results indicated that proper history taking affected the patient’s emotional status, whereas patient education demonstrated to affect physical health level of function, blood pressure, and blood glucose levels. Having a detailed history was found to truly have a significant association with patient outcome; so be sure to ask a wide range of questions not only about physical aspects but feelings and concerns, understanding the problem, expectations of therapy, and perceptions of how the problem affects function.
Reduced chances of lawsuits with better communication

Medical malpractice premiums in the United States total more than 5 billion annually, so if better communication can help in reducing the probability of being taken to court for a misunderstanding why not do so? Quality of care alone was a poor predictor of medical malpractice claims — rapport between patient and physicians was found to be a principal determinant.
Physicians who exhibit more negative communication behaviors are more likely to have been sued. Positive patient-doctor relations increases patients’ perception of physician competencies, decreases perception for physician responsibility for an adverse medical outcome, and decreases their expressed intentions to file malpractice claims.
Learn to sit down

The patients commented how appreciative they were and how grateful that the doctor took the time to “sit and listen” (O’Callaghan, 2010). The perception was only 61% positive when the physician was standing with comments such as, “I didn’t have the time to ask the doctor any questions” and “he was in and out” being common sentiments (O’Callaghan, 2010). Overall improving patient communication can lead to better patient compliance with doctors’ orders, lower levels of litigation and decrease in unnecessary costs – it is a small gesture that can greatly enhance the patient care experience.
Patient vs. Doctor
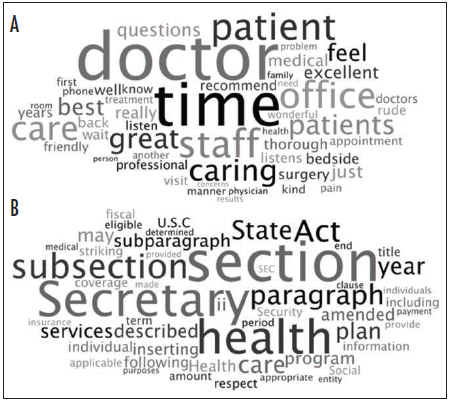
While patients and physicians agree on what constitutes competent communication skills, they disagree on whether their physician possesses this skill. So essentially doctors are from Mars and patients are from Venus when it comes to communication in that doctors agree more closely with one another compared to their patients.
What we’re seeing is that while you may think you are consistent with your communication skills from patient to patient, your patients disagree and they have no uniform consensus. And while you may think you communicate better than that know-it-all peer of yours, you’re no different than they are per your patients’ evaluation. So don’t be a jerk and be nice, even if the patient deserves a few good choice words – it could save everyone, especially you, some money in the long run and ensure your reputation remains intact.
Conclusion:
At the end of the day it is about the patient and ensuring they find relief in their time of need; so if communication is one of the barriers stop by planet Venus – I’ve heard it’s not that bad just a little windy.
Guest author: Ivanna Liberato is an IT Systems Administrator pursuing a degree in Cognitive Neuroscience who enjoys dabbling into the art of blogging via her blog Yes I’m Crazy, That’s Why I’m Awesome.
Images from: www.androidpit.com,www.dreamstime.com,csalner.wordpress.com,www.ankota.com