AI in Action: Outpatient Clinics: What’s Really Working (and What’s Not) in 2026
Walk into almost any outpatient clinic in 2026, and you’ll feel the shift. Check-in moves quicker. Imaging results show up while the visit is still fresh. Follow-ups don’t feel like an afterthought.
AI is no longer a pilot. It’s part of the routine, and it’s starting to reshape patient access in ways that are immediately visible at the front desk.

That shift traces back to moments that made AI usable in real settings. FDA clearance of systems like Eyenuk’s EyeArt in 2020 did exactly that, proving autonomous screening for diabetic retinopathy could work inside everyday clinical workflows. From there, progress has been steady. Imaging tools have improved. Predictive models became more usable. Language systems found their way into notes, messages, and intake.
Now the question isn’t whether AI belongs in outpatient care. It’s where it actually helps, and where it still creates friction. This article breaks down what is working today, where clinics are struggling, and what to watch as adoption continues.
Current Applications of AI in Outpatient Clinics
AI is showing up across different parts of the clinic, but not all use cases carry the same weight. Some improve speed without changing outcomes, while others quietly reshape how care is delivered. Here’s where it’s making a measurable difference right now:
1. AI in diagnostics and patient assessment
Imaging is where AI proves itself fastest.
Retinal scans are reviewed within minutes, not days, which means patients get screened during the visit rather than being sent elsewhere and hoping they follow through. In breast cancer screening, AI-supported workflows are reducing radiologist workload without compromising safety, which matters when clinics depend on limited reading capacity.
That’s where the value shows up first—faster answers. Fewer missed follow-ups.
Outside imaging, predictive models are flagging patients at risk of falls, readmissions, or gaps in care. When those signals are actually used, clinics intervene earlier. When they’re ignored, nothing changes.
AI as a “second set of eyes” sounds simple. In practice, it catches edge cases. Subtle patterns. The kind that get missed when clinics are running behind. That’s where confidence improves, and where clinicians spend less time double-checking and more time deciding what to do next.
2. AI in administrative tasks and workflow management
The back office is where AI quietly delivers.
Scheduling systems now anticipate no-shows and prompt patients before slots are wasted. Referral notes are cleaned up and routed correctly, avoiding bounces between departments and improving referral management in busy, multi-specialty environments. On the revenue side, eligibility checks and claim edits are handled before submission, not after rejection. The CAQH Index continues to point to billions in avoidable administrative costs.
This isn’t flashy work. It’s necessary work.
When it’s done well, staff stop chasing paperwork. They spend more time dealing with exceptions, not routine tasks. Multi-site clinics feel this the most—less manual coordination. Fewer dropped steps.
The difference shows up in small ways. Fewer rescheduled visits. Fewer billing surprises. Less friction overall.
Nick Wiese, Regional Vice President of Alpha Heating & Air, oversees operations where timing, coordination, and clear workflows directly affect service delivery.
He says, “The biggest gains don’t come from adding more tools. They come from removing friction in the handoffs. When scheduling, routing, and follow-ups are aligned, teams stop reacting and start operating with intent.”
3. AI in personalized patient care
Personalization is where patients tend to feel the difference.
Reminders arrive when they’re actually useful. Education is clearer, not buried in medical jargon. Basic questions get answered without waiting on a callback. Chatbots handle simple interactions before and after visits, shaping the overall patient experience before a clinician even enters the room.
Pair that with remote monitoring, and patterns start to surface. Subtle changes. Early signs of deterioration. Clinics can act before the situation escalates.
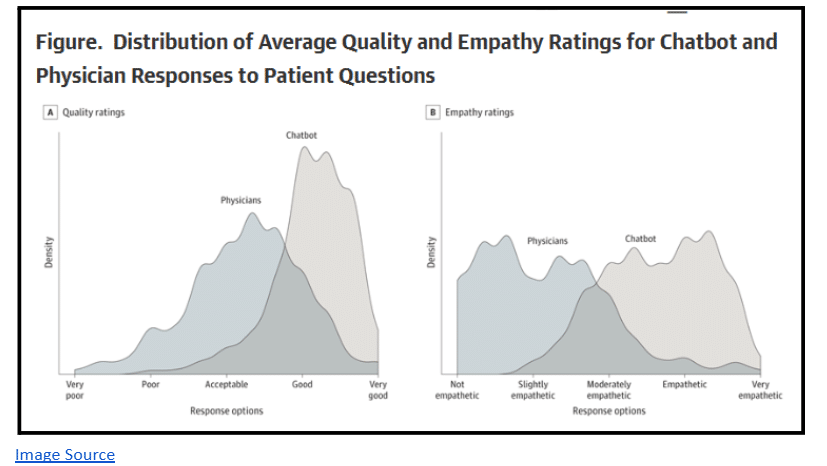
Tone matters more than expected. In one study, AI-generated responses were sometimes rated as more empathetic than physician responses. That says less about AI and more about how communication is delivered at scale.
Efficiency helps. But patients still respond to clarity and empathy.
The strongest setups use AI to handle volume so clinicians can focus on conversations that actually require judgment.
Success Stories: What’s Really Working in 2026
Not every implementation delivers results, even when the technology is solid. The difference usually comes down to how focused the rollout is and whether the workflow around it actually supports it. These are the patterns showing up in clinics that are getting real value:
1. Case studies of efficient AI integration
The clinics seeing results aren’t doing more. They’re doing less, but better.
They focus on one workflow. One problem. Something measurable.
Before rolling out anything new, they fix the basics. Data quality. Identity matching. EHR integration. Without that, even good tools fail.
Then they train their teams properly. Not once. Continuously.
In practice, this shows up in specific ways. An imaging AI tool that feeds structured results directly into the clinical note. A scheduling system that predicts no-shows and suggests safe overbooking ranges.
Nothing broad. Nothing abstract.
Tight scope makes it easier to see if it actually worked.
Having worked closely with teams rolling out new systems inside existing operations, Eric Yohay, CEO and Founder of Outbound Consulting, often sees where implementation efforts lose traction.
“The pattern is pretty consistent. The teams that try to do too much upfront struggle to show any real progress. Those who pick a single workflow and stay focused on it tend to move and learn faster. That early clarity makes scaling much easier later on,” Yohay notes.
2. AI’s impact on patient outcomes and clinic performance
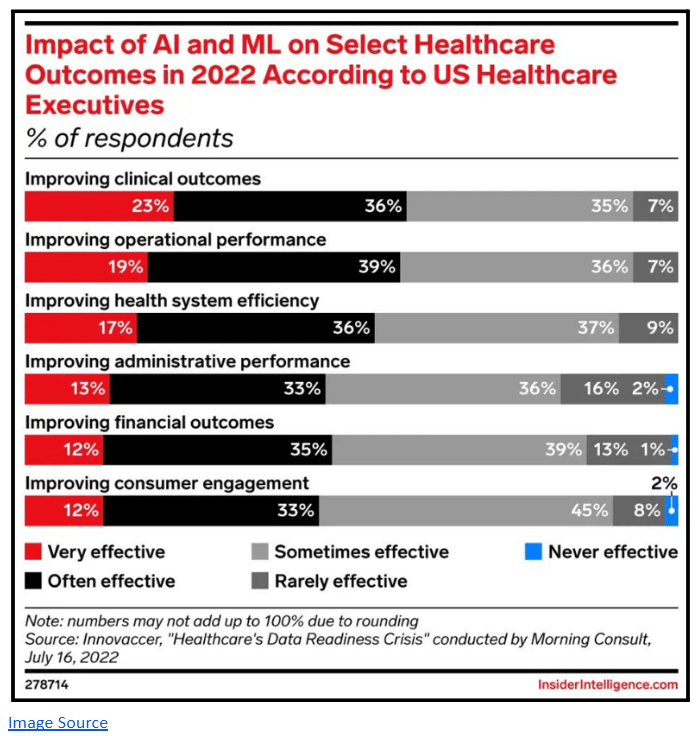
In a 2022 study by Innovacer, 36% of US healthcare leaders called AI/ML consistently effective at boosting clinical outcomes—39% for operations and 36% for system-wide efficiency.
These beliefs underpin the measurable gains now materializing.
AI-supported mammography workflows reduce workload without compromising safety, helping clinics move through backlogs. Autonomous retinal screening increases same-day detection. Administrative automation continues to reduce time and costs for repetitive transactions.
The operational impact is measurable and largely driven by the growing maturity of healthcare technology that fits into existing workflows rather than disrupting them.
The human impact is easier to miss, but just as important.
Clinicians spend less time documenting. Ambient tools summarize visits and draft notes in the background. Patients get answers faster, with fewer handoffs.
Less noise. More focus.
That’s where the value compounds.
Challenges and Limitations: What’s Not Working
For all the progress, there are still points where things stall or break down. Most of the issues aren’t obvious at the start, and they tend to surface only after rollout. These are the areas where clinics are still running into friction:
1. Technical and operational challenges
AI breaks down when the data does.
If systems don’t talk to each other, outputs become unreliable. Duplicate records, delayed updates, incomplete histories. Even with modern APIs, clean data still takes work.
This is where the underlying healthcare IT infrastructure begins to show its limits, especially in clinics that still rely on fragmented or outdated systems.
Then there’s drift. Models shift over time as patient populations and workflows change. Without monitoring, performance quietly degrades.
Healthcare systems remain high-value targets, and breaches involving third parties have doubled from 15% to 30%, showing how quickly risk expands when external vendors are introduced into the ecosystem. As more AI tools rely on integrations, APIs, and external platforms, each additional connection becomes another potential point of failure that clinics don’t fully control.
Predictive models, too, including sepsis detection systems, have underperformed in real-world settings, missing cases or creating false alarms that erode trust.
Validation can’t be skipped. Neither can ongoing oversight.
2. Ethical and human aspects
AI can guide. It cannot replace judgment.
Clinical decisions still depend on context. Patient history. Trade-offs that no model fully captures.
Bias remains a risk. If historical data reflects disparities, outputs will mirror them unless actively corrected.
Patients are paying more attention to this.
They want to know when AI is involved, how it’s used, and what happens to their data. Clear communication matters. So does restraint. Not every task should be automated.
Ryan Beattie, director of business development at UK SARMs, works closely with individuals navigating decisions where outcomes carry long-term weight.
He puts it: “Based on what I’ve seen, people are open to technology being part of the process. But when it starts to feel like it’s replacing judgment, that’s where hesitation comes in. Especially in situations tied to health, people want to know there’s still a human responsible for the final call.”
3. Economic and regulatory barriers
Costs extend beyond the tool itself.
Integration work. Staff training. Workflow redesign. These add up quickly, and they’re often underestimated.
Many projects stall here. Not because the technology fails, but because the groundwork wasn’t planned.
Regulation adds another layer. Frameworks continue to evolve, and clinics have to keep up without slowing down operations.
That includes guidance from the FDA on AI-enabled medical devices, interoperability requirements under the 21st Century Cures Act, and CMS efforts to streamline prior authorization through APIs.
The direction is clear. The details are still shifting.
Looking Forward: Future Trends in AI for Outpatient Clinics
The next phase looks more practical.
Instead of one large system trying to do everything, clinics are adopting smaller, purpose-built tools. Many run locally, keeping sensitive data closer to the source and easier to validate.
Ambient systems will continue to improve. Listening, summarizing, and coding, all without interrupting the visit.
Privacy-focused approaches like federated learning and synthetic data are gaining traction. They allow models to improve without centralizing sensitive information.
Operationally, AI will start handling more of the prep work and verifying requirements and assembling documentation and identifying the fastest referral paths.
Some of the slowest parts of care will finally move.
Frameworks like NIST’s AI Risk Management Framework are giving clinics a way to standardize oversight and reduce uncertainty.
The tools are improving. But the difference will come from how they’re used.
Navigating the AI Pathway in Outpatient Clinics
AI is already part of how outpatient clinics operate.
The wins are visible. Faster diagnostics. Less administrative friction. Clearer communication with patients.
The gaps are just as real. Data issues. Model drift. Bias. Costs that show up later.
Progress depends on restraint.
Start with one problem. Make sure the system around it works. Involve the people who use it every day. Adjust when it doesn’t fit.
Keep decisions where they belong with clinicians.
When AI handles the routine, time opens up for everything else.
If you’re looking at how to make these systems work in practice, explore how clinics are streamlining workflows with ReferralMD.
Author’s Bio: Catherine is a marketing & e-commerce specialist who helps brands grow their revenue and move their businesses to new levels.